Table of Contents
Rheumatoid arthritis (RA) is an autoimmune disease in which the body’s immune system is triggered to attack tissues, joints, and cartilage. More than 1.5 million in the United States suffer from rheumatoid arthritis. A person with RA can experience extreme pain, inflammation, swelling, and stiffness.
As RA progresses, its symptoms can worsen. The disease can affect not only the joints but the cartilages as well, which may result to permanent damage and loss of function. Additionally, complications may arise as the inflammation spreads to the tissues of the heart, lungs, kidneys, skin, and eyes.
There is currently no known cure for RA, though its symptoms can be effectively managed by a variety of treatment options. Currently, studies are being done to look at other alternatives, one of which is stem cell therapy.
What Is Stem Cell Therapy?
The human body has over 200 different types of cell, each having definite characteristics that allow them to perform clearly defined roles. Cells with the same roles group together to create tissues, which then form organs. For instance, muscle tissues cluster together to create the heart.
Stem cell therapy is a procedure in which a person’s dead and diseased cells within the body can be replaced with healthy ones. A stem cell is a type of cell with no specific function; instead, it possesses the unique ability to adapt and develop into various types of cell as the situation requires.
The Process
The stem cells are sourced from body tissue, which can come from either an embryo or an adult human. The stem cells are isolated in the laboratory and are then controlled and regulated to develop into specific cell types. Once done, these cells are injected into the person’s tissue or blood stream.
There had been debates over the ethical and moral considerations in stem cell therapy, as these stem cells were harvested from a separate specimen. However, advances in technology and medicine are rendering these debates null. Indeed, the cells for this procedure can now be replicated within the person’s own body. Since their own cells are involved, the risks could be considerably lessened, as opposed to when cells from another person is used.
How Stem Cell Therapy Can Help with Rheumatoid Arthritis
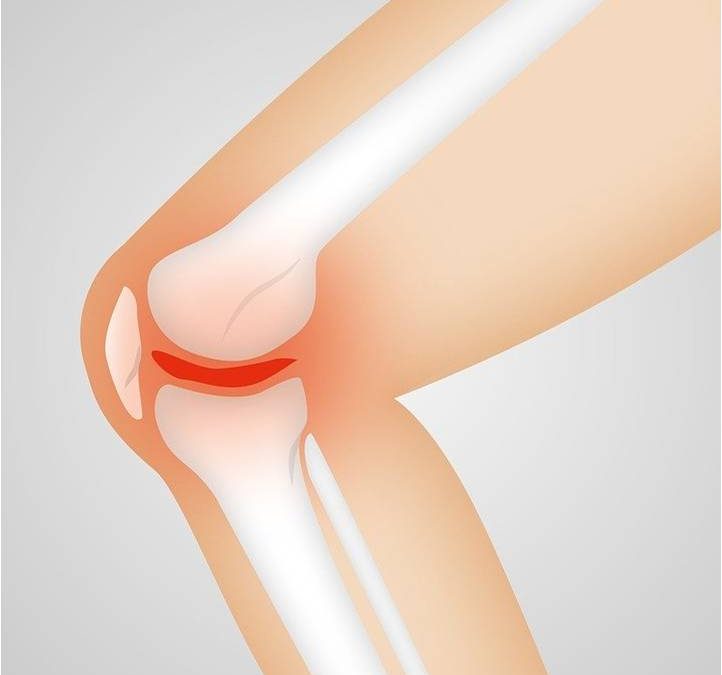
In RA, the immune system attacks the lining of the joint capsule. This leads to the inflammation of the joints, leading to chronic pain and swelling. As the disease progresses, the cartilage, which is the connective tissue between joints, deteriorate as well.
With stem cell therapy, the cells in the cartilage and bones are replaced using mesenchymal stem cells (MSCs). MSCs are injected into the tissues surrounding the affected joints. Aside from replacing the diseased cells, this could potentially reduce the inflammation caused by the immune system.
Where operation logistics are concerned, MSCs lessen the worry for Human Leukocyte Antigen (HLA) matching. MSCs derived from umbilical cords are not recognized by the immune system as a foreign body, and thus cell rejection won’t be a problem.
Is Stem Cell Therapy an Effective Treatment Option for Rheumatoid Arthritis?
Stem cell therapy is a promising alternative treatment for RA. However, since it is still in its trial stage and research studies are still limited, it is far from being standard practice for RA treatment. More analysis will have to be done to investigate its effectiveness both in the short-term and long-term recovery of the patient.
Risks and Side Effects of Stem Cell Therapy
Because of the limited resources and studies done on the subject with respect to using it as a viable treatment option for RA, stem cell therapy can cause some medical complications.
Some of these complications may include:
Infections
Injecting cells into the body, and using harvested cells in the first place, makes the specimen susceptible to contamination especially when not handled properly enough. Viruses and bacteria may interact with the specimen, and thus enter the body without resistance. These harmful microbes may cause an infection to develop or may even worsen an existing infection.
Worsening of Rheumatoid Arthritis
Though stem cell therapy may be done to treat RA, there is still the risk of it aggravating the symptoms of the disease instead. Not enough studies have been done to fully conclude the scope of its effects on the treatment of RA.
In Summary
Most research on stem cell therapy is still on the inception or clinical trial stage. They offer promising insights on the effectivity of stem cell therapy as a treatment for RA in the future, but right now, it is far from being a sustainable standard procedure. Further work would have to be done by scientists to advance this idea.
Additionally, studies on the cause behind the immune system attacking its own cells, tissues, and organs are also being done to get to the root of autoimmune diseases like RA. This question, should it be answered, would be instrumental in understanding autoimmune diseases and in developing far more effective treatment options than those at hand right now.


 I love to write medical education books. My books are written for everyone in an easy to read and understandable style.
I love to write medical education books. My books are written for everyone in an easy to read and understandable style.