Table of Contents
In most cases the pain associated with degenerative disc disease is episodic, presenting in brief, acute flare ups. These episodes may go on for years, however, so it’s still important to master techniques for coping with chronic pain.
Stress Reduction
Most of the techniques discussed here have a central goal of releasing stress and counteracting negative feelings that may range from anger and impatience to anxiety, sadness, frustration, and depression.
No two people will respond equally to the same relaxation techniques, so don’t give up. If a technique like guided imagery doesn’t let you craft a mental escape, but beautiful music calms your mind and relaxes your body, then stock up on CDs and download MP3s to your heart’s content!
Whatever works, use it!
Some Things That Don’t Work
Having a stiff drink — or several — when you’re in pain may seem like a good idea, or even a culturally acceptable way to take the edge off. The physiological truth, however, is that alcohol has a depressive effect on your mood, it inhibits nerve activity in the body, slows healing, and interferes with sleep.
None of those things are going to help you really manage your pain.
Endorphins, Natural Drug of Choice
Instead of using alcohol, find some exercise you can do — even just taking a walk — to get your body’s own feel good drugs, endorphins pumping. Endorphins are peptides secreted by the brain that have an analgesic effect because they stimulate opiate receptors in the body.
That runner’s high? That notion of “hitting the wall” and then feeling better? It’s real. You don’t have to run a marathon to get a “hit” of endorphins. For most people a nice brisk walk in the fresh air will do the same thing.
If you’re not the outdoors type? Get on the treadmill or even a stationary bike. You will feel better afterwards.
Practice Deep Breathing
Holding your breath or breathing very shallowly is a common reaction to chronic pain. This causes a build-up of tension, tightening the muscles of the body and making the pain worse. Deep breathing is a good technique to release that tension. An added benefit is increased blood flow and oxygenation, which facilities healing.
Meditation experts recommend visualizing a balloon in the stomach. As you breathe in, fill the balloon. Put your hands on your stomach so you can feel the air moving into the balloon. Exhale just as deeply, deflating the balloon just as you filled it.
You can practice this technique anywhere, but at least once or twice a day, try to find a quiet spot and really get comfortable. Use your deep breathing as a form of meditation to settle your thoughts and take a break for a few minutes.
Don’t Concentrate on the Pain
The more you think of your chronic pain, the more you will hurt. It’s crucial to find some activity that completely absorbs your mind. Concentration is a powerful pain reliever, especially when you’re doing something you enjoy. If you don’t have a hobby or an all-consuming project, find one!
Keep a Pain Journal
While the suggestion to keep a pain journal may seem to contradict the advice not to focus exclusively on the pain, it’s important to understand all kinds of situations that make your pain worse.
In the case of a bad back, this may be how you’re sitting, or even the weight of your briefcase in your hand on the way to the office.
It may be more illuminating, however, when you realize that your pain is worse after a tense conversation with your boss because you’re tense. That’s when some deep breathing is in order.
Tracking your pain allows you to find your triggers and either head them off in advance, or be prepared to deal with them in the aftermath.
Be Kind to Yourself
Some days will be better than others. There will be times when you need the painkillers, or when staying on the heating pad is all you want to do. It’s okay to indulge those feelings for a day or two, but you can rest a bad back too much and wind up with an even more debilitated state.
It’s okay to be patient with yourself and kind, but realize that living with chronic pain is an active process that involves both the mind and the body.
Epidural injections paired with some type of numbing agents are intended to both relieve back pain and to decrease inflammation.
The shots do not work uniformly for all patients, but they are particularly well suited to the sharp pains typical of nerve damage in the neck and lower back.
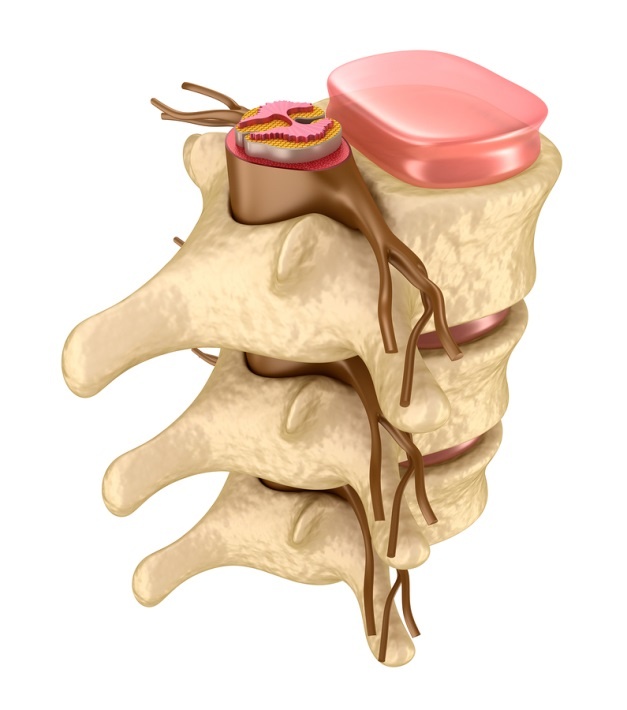
This “radiculopathy” typically originates at the point at which a nerve exits the spine. Epidural injections target the epidural space, the area lying between the spine’s protective covering and the vertebrae themselves.
Epidural injections are also useful in cases of spinal stenosis, which is a narrowing of the spinal canal causing compression of the spinal cord or its adjacent nerve structures.
Typically an epidural is performed as an out-patient procedure at a doctor’s office by an anesthesiologist or radiologist.
The procedure is a simple one, involving the guided insertion of the needle using a live X-ray or fluoroscope. This allows the doctor to correctly position the needle for the placement of the corticosteroid medication.
Since a numbing medication is used first, the injection is not usually painful, although the site may be tender for a few days afterwards.



 I love to write medical education books. My books are written for everyone in an easy to read and understandable style.
I love to write medical education books. My books are written for everyone in an easy to read and understandable style.