CHAPTERS
Navigate to chapter
► Chapter One: Deeper Look at Psoriatic Arthritis
► Chapter Two: Signs, Symptoms and Complications
► Chapter Three: Treatment and Management
► Chapter Four: Dealing with Psoriatic Arthritis Naturally
► Chapter Five: How Changing Your Diet can Affect Psoriatic Arthritis
► Chapter Six: Living with Psoriatic Arthritis
► Chapter Seven: Get Some Motivation
Chapter One: Deeper Look at Psoriatic Arthritis
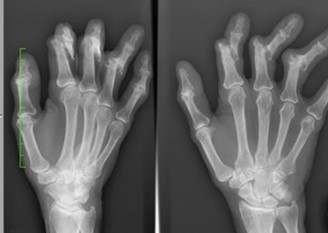
Having psoriatic arthritis is a very difficult condition. Not only do you have to deal with the symptoms of psoriasis, but you also suffer from the almost unbearable effects of arthritis. All the stiffness, swelling and discomfort in the joints can not only disrupt your daily life, but also bring tremendous amount of pain. Psoriatic arthritis is a progressive autoimmune disease. What is an autoimmune disease?
The human body has an immune system that is designed to protect itself from the onslaught of infection and disease. However, there are cases when the cells in the immune system attack healthy cells in other parts of the body by mistake—this is called autoimmune disease. There is no known cause for psoriatic arthritis just as it is not clear why autoimmune diseases develop. It is unknown as of yet why the immune system will fight healthy tissues. But the condition is likely to run in families, particularly women.
Environmental factors and physical trauma also play a vital role in the condition. The disorder in one’s immune system can bring about a lower or higher rate of activity wherein tissues are damaged and the body’s natural ability to ward off diseases suffer, thereby causing the body to be vulnerable to illnesses and infections. There are about 80 different kinds of autoimmune diseases and a classic symptom is inflammation. Inflammation of different kinds of body tissues can cause pain, swelling, heat, and redness, which can result in muscle aches, low fever or fatigue.
Autoimmune diseases also flare up, meaning the condition gets worse and the patient suffers remissions. The main goal of addressing autoimmune diseases is to lessen the inflammation.
As with any autoimmune disease, the symptoms of psoriatic arthritis can appear or disappear anytime. You may think that you are getting better only to suffer another, more sever flare-up of the skin and joints. Psoriasis can affect the scalp, navel, ears, knees, elbows, and even the genital areas. This inflammation of the skin is prevalent, affecting about 2% of the population of Caucasians in America. Similarly, about a quarter of patients who suffer from psoriasis can develop inflammatory arthritis.
According to studies, psoriatic arthritis begins to show in the 40s or 50s, and both males and females can be affected. The problem of skin inflammation and joint inflammation can appear separately, and usually psoriasis is the first diseases that almost 80% of people have to deal with first. In cases where the inflammatory arthritis appears first, doctors find it difficult to diagnose correctly until they develop psoriasis. In cases like this, the joint problems begin even before lesions in the skin appear.
Patients who suffer from psoriatic arthritis suffer similar symptoms of different systemic rheumatic diseases and arthritic conditions such as Crohn’s disease, reactive arthritis and ankylosing spondylitis where there is inflammation of the joints, spine and some organs of the body like the heart, kidney, lungs and eyes.
As with any autoimmune disease, the cause for psoriatic arthritis remains unclear. Genetics, environmental factors, family history and even physical trauma can contribute to the development of the condition. For instance, a bacterial infection can trigger the disease in people that have an inherent tendency. Following are the risk factors that can increase the possibility of developing psoriatic arthritis:
- Psoriasis. People who already have inflammation of the skin have a great chance of developing psoriatic arthritis, especially when they begin to have lesions on their nails.
- Genetics and family history. According to research, people who have relatives in the first degree that have psoriatic arthritis have a tendency to develop the illness as well.
- Age. Psoriatic arthritis tends to occur more prominently in people aged 40 to 50. Nevertheless, the condition does not only occur in this age group, anyone can acquire psoriatic arthritis.
People with psoriatic arthritis can suffer from complications. One of the most severe complications is called arthritis mutilans. This is a harsh, agonizing, immobilizing form of psoriatic arthritis. Arthritis mutilans will destroy the little bones like the fingers. The patient will then be disabled and deformed.
Another complication is the pinkeye or conjunctivitis. This can cause reddened eyes, blurred vision, and pain in the eye area. Depending on their genera health and the progression of the disease, some patients with psoriatic arthritis can even develop cardiovascular diseases.
You can learn more about the different signs and symptoms of psoriatic arthritis in the next chapter. If you already have psoriasis and you start to experience joint pain, be sure to inform you doctor immediately. Early diagnosis and treatment can help you manage the condition. If untreated, the condition can relentlessly damage your joints. It is never too early to get proper treatment; it can save your life.
Continue Reading…
Want to read the entire thing?

